Dr. Nimesh Patel
Dr Nimesh Patel has an outstanding academic record. He did his MBBS & MS-General surgery from the prestigious SSG hospital & Baroda Medical College. He did his DNB – Neurosurgery from the prestigious Amrita Institute of Medical Science, Kochi, Kerala. Following completion of Neurosurgery, he joined as a faculty in the same institute. He is specialised in Neurooncology, Neurovascular & Spine surgeries in which he did his fellowships. He is very well trained for minimally invasive spine surgery along with spine tumor surgeries. He has vast experience of Neuronavigation guided, Stereotactic and Endoscopic brain surgeries.
Back Pain
`Back Pain` is one of the commonest complaints doctors come across nowadays. When you feel pain, it is really a reaction to signals transmitted throughout your body. These signals are sent from the pain source — such as a sore back, through the nerves in the spinal cord, and up to the brain, where they are perceived as pain.
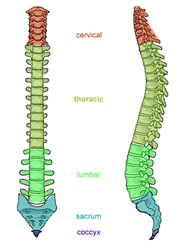 Our Spinal Column Our Spinal Column |
Different Types of Pain
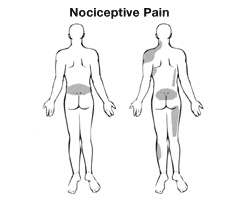
The origin of some pain is neuropathic, while other pain is nociceptive. This is important to know because different treatments work better for each type of pain.
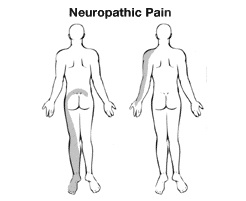
Neuropathic pain is caused by damage to nerve tissue. It is often felt as a burning or stabbing pain. One example of neuropathic pain is a “pinched nerve.”
Nociceptive pain is caused by an injury or disease outside the nervous system. It is often an ongoing dull ache or pressure, rather than the sharper, trauma-like pain that is characteristic of neuropathic pain. One example of nociceptive pain is arthritis pain.
Some people experience mixed pain, which is a combination of neuropathic and nociceptive pain.
 |
 |
Chronic versus Acute Back Pain
Chronic back pain is commonly described as deep, aching, dull or burning pain in one area of the back or traveling down the legs. Patients may experience numbness, tingling, burning, or a pins-and-needles type sensation in the legs.
Acute back pain is commonly described as a very sharp pain or a dull ache, usually felt deep in the lower part of the back, and can be more severe in one area, such as the right side, left side, center, or the lower part of the back. Acute pain can be intermittent, but is usually constant, only ranging in severity.
Sometimes, acute back pain can be caused by injury or trauma to the back, but just as often has no known cause. Patients with acute back pain, even when it’s severe, will typically improve or completely recover within six to eight weeks.
Approximately half of all back pain patients have acute pain caused by trauma. A contusion, torn muscle, or strained joint resulting from a back injury can cause acute pain. Patients with any of these conditions typically exhibit pain, muscle spasms, and decreased functional activities. Treatment of acute back pain is short-term and usually successful. With physical therapy, follow-up treatment, and prevention practices, these patients typically return to full functionality in a few weeks. Occasionally, these patients will re-injure themselves and have to return for a short course of treatment. Patients with acute pain occurring more than three times in one year or who experience longer-lasting episodes of back pain that significantly interfere with functional activities (e.g., sleeping, sitting, standing, walking, bending, riding in or driving a car) tend to develop a chronic condition.
Mechanical back pain—a form of acute pain—is aggravated by movement and worsened by coughing. This type of pain is usually alleviated with rest. Mechanical back pain is typical of a herniated disc or stress fracture. For patients with this condition, forward movements of the spine usually cause pain. In addition, posture, coughing, sneezing, and movement can all influence pain coming from the spine.
WARNING SIGNALS (red flags to identify a serious underlying problem)
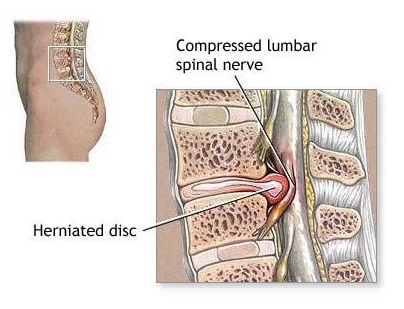
- Pain radiating down from the back or the neck to the lower or upper limbs, respectively. This would be more significant if the pain aggravates on coughing/ sneezing/ certain movements of the back or the neck. This pattern of pain would generally indicate a disc herniation or related problem.
- Weakness or numbness in a specific part of the hands or legs. This might indicate a nerve getting “pinched” n the spine.
- Unsteadiness while walking. Though there are a host of problems that can lead to this kind of presentation, one of the foremost and also, one of the treatable causes is compression of the spinal cord in the neck or upper back region.
- Pain in the calf or buttocks on walking or standing for some time and getting relieved on sitting down or stooping forwards. This would indicate a pathological spinal condition termed “spinal canal stenosis”.
- Deformity of the back or a bony hump seen on one side of the midline of the back. This could indicate a spinal deformity which would have the best treatment results if detected early.
Investigations for Acute Back Pain
- X-rays—Painless, non-invasive imaging process that utilizes photographic film to absorb electromagnetic radiation—having an extremely short wavelength of less than 100 angstroms and the ability to penetrate solids of various thicknesses—transmitted through a material body. These images, also known as radiographs or roentgenograms, are used to diagnose and monitor the treatment of various disorders.
- CAT Scan (computed axial tomography scan)[also called a CT scan (computed tomography scan)]—Another painless imaging technique that utilizes a computer to produce detailed three-dimensional images of a body from a collation of cross-sectional X-rays taken along an axis. Of all the imaging techniques that are currently available, the CAT scan is best able to produce images of bone, blood, and soft tissues.
- MRI (magnetic resonance imaging)—Non-invasive technique for imaging the spine that involves rotating a magnet around the body and exciting its hydrogen atoms. A scanner is then utilized to detect the energy emitted by the excited atoms. MRIs provide exceptional detail of the spine’s anatomy, since the human body is composed primarily of water, which is two parts hydrogen. The single most useful test available for diagnosing spinal disorders.
- Myelogram—A test procedure that involves injecting a radiographic contrast media (dye) into the sac (dura) surrounding the spinal cord and nerves, and then taking X-rays of the spine. This allows the radiologist to specifically X-ray the nerve roots. In this way, any abnormalities within the spinal canal can potentially be identified to aid in the diagnosis of certain spinal problems, such as nerve compression or a disc rupture.
- Bone Scan—A test procedure that involves intravenously injecting a small quantity of a radiographic marker into the patient, and then running a scanner over the area of concern. The scanner detects the marker, which concentrates in any region exhibiting high bone turnover. A bone scan is utilized when there is suspicion of tumor, infection, or small fractures, i.e., conditions that all result in high bone turnover. A Bone Scan does not replace the above tests, but
Types of spine surgery
Different types of spine surgery include:
- Diskectomy. This involves removal of the herniated portion of a disk to relieve irritation and inflammation of a nerve. It’s done as an open surgery and typically involves full or partial removal of the back portion of a vertebra (lamina) to access the ruptured disk.
- Laminectomy. This procedure involves the removal of the bone overlying the spinal canal. It enlarges the spinal canal and is performed to relieve nerve pressure caused by spinal stenosis.
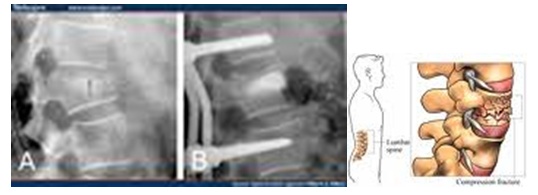
- Fusion. Spinal fusion permanently connects two or more bones in your spine. It can relieve pain by adding stability to a spinal fracture. It is occasionally used to eliminate painful motion between vertebrae that can result from a degenerated or injured disk.
- Vertebroplasty. During this procedure, your surgeon injects bone cement into compressed vertebrae. For fractured and compressed vertebrae, this procedure can help stabilize fractures and relieve pain. With a similar but more expensive procedure — called kyphoplasty — a balloon-like device is inserted to attempt to expand compressed vertebrae before bone cement is injected.
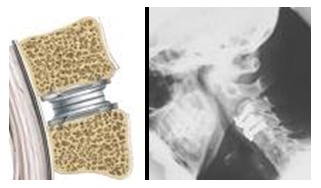
- Artificial disks. Implanted artificial disks are a treatment alternative to spinal fusion for painful movement between two vertebrae due to a degenerated or injured disk. These relatively new devices are still being studied, however, so it’s not yet clear what role they might play in treating spinal disk disease.
FAQ s related to Spine problems :FAQ s related to Spine problems :
What is slipped disc?
Our back is made up of small bones piled up one and other with intervening soft cushions known as intervertebral discs or discs for short. These discs are soft structures with balloon like tendencies, i.e. they are tense and pressurized.When the disc (balloon) ruptures the contents go out of place and in the process cause back pain or pain in the legs (or in the arms and hands in case of neck problems) if it happens to irritate or cause pressure on nerves that pass nearby it.
What is Sciatica?
“Sciatica” is a very broad term used to describe radiating pain in the legs which is due to some problem with the leg nerves originating in the back. The usual problem is some kind of pressure due to a slipped disc or nerve pressure due to a variety of other causes.
Is Sciatica treatable?
Yes, it is definitely possible to treat sciatica in majority of the cases. The common reasons are some form of pressure on the nerves in the back. If the cause can be diagnosed by investigations it is usually possible to treat it.
What is spondylosis/spondylitis?
Spondylosis or spondylitis, which are commonly used terms only mean that the back is undergoing an age related degeneration. It means “wear and tear”. It is not something to be feared because aging affects each and every one of us. It is only in some individuals this can lead to pain and other problems, which can are treatable.
Is it necessary for a person with back pain to sleep on a hard surface or floor?
No, the common notion that a person having back problems must sleep on a hard board or on the floor is not correct. One can certainly use a mattress which is firm enough. A mattress of coir is probably the best. Cotton mattresses which develop uneven surfaces and the very soft cushioned mattresses in which the body sinks inside are better avoided.
What complaints in the legs should alert one to the possibility of back problems?
Any pain in the legs which seems to be starting from the back or the buttock region and traveling into one or both the legs. Along with the pain there may be a feeling of “pins and needles” or tingling and numbness in parts of the leg. One may find some weakness in the affected leg in the form of heaviness or difficulty while walking. In the middle aged and elderly there are typical symptoms whereby the person feels pain , heaviness, tingling, numbness and weakness in the legs which increases on walking or standing and is relieved by sitting or bending forwards. These complaints are also related to nerve compression in the back and can be treated by medicines, exercises and in extreme cases by surgery.
What are the restrictions in the lifestyle of people with back problems?
As a spine surgeon, I would try to put minimum restriction on the lifestyle of any back pain patient especially if the person is young and active. If a person is suffering from a back problem the general precautions include avoid frequent bending (occasional bending is allowed), not to bend and lift (lifting should be done using the knees), not to lift very heavy objects, not to sit continuously for a prolonged period, sit on a proper chair, avoid sitting down on the ground. The restrictions put significant brakes to the person’s life, I would offer a surgery if it is possible to make the person’s life less restricted.
What causes neck pain and why is seen so commonly these days?
Our neck is a very delicate piece of architecture which has a very high mobility and a tendency to be misused. Occupations involving excessive use of neck lead to neck pain and neck problems. These include computer professionals, persons using computers extensively, telephone operators and person having to write for several hours. Wrong sleeping position, using a very big pillow or no pillow or frequently sleeping in sitting posture with the neck unsupported can lead to neck problems.
Under construction..